Lupus — the most common cause of congenital heart block, the leading cause among young women of premature cardiovascular disease, kidney disease, and stroke — leaves clues for detection in your skin.
By Emily Jorge, DCNP, FNP-BC
What is most common cause of congenital heart block? [1]
What is the leading cause of premature cardiovascular disease, kidney disease, and stroke among young women?
What affects 1.5 million Americans and is three times more prevalent in women of color?
Did you know the first therapy in 50 years was approved for this disease in 2011?
Just 20 years ago, only 40 percent of people were expected to live more than three years with this diagnosis. [2]
Lupus.
No single test can determine if a patient has this. Typically it requires a combination of several laboratory tests with clinical assessment. It can be difficult to treat depending on which type it is, severity of disease, and individual response. There are several variants of lupus. Here are four types we will look at:
- Neonatal Lupus: Skin lesions are usually present at birth but may appear several months later. We are unsure of the cause, but believe antibodies passed from the placenta play a role. [2] The three potential systemic findings other than a rash are congenital heart block, hepatobiliary disease and low platelets–a condition we call thrombocytopenia. There is a 20 percent mortality rate associated with cardiac neonatal lupus and some children require pacemakers as a result. Neonatal lupus usually resolves by 12 months of age, but the cardiac effects (such as conduction problems and structural abnormalities) continue. [3]
- Discoid Lupus: Skin lesions are most often found on the head and neck, occasionally on mucosal surfaces. The presence of lesions below the neck can occur, usually in conjunction with patches or plaques above the neck simultaneously. Discoid lesions have the potential to scar which may lead to disfigurement of the individual. Hair loss with scarring and pigment changes are common. Some references cite the incidence of progression to systemic lupus as low as 1-5 percent and others 5-15 percent. Those with more widespread lesions are thought to have more risk of progression. Sun exposure seems to promote lesion development. [3]
-
Subacute Cutaneous Lupus Erythematosus: The distribution is typically on sun-exposed areas and can range from being mild, with only a few patches to involving the upper body. These lesions may lead to pigment changes, but do not scar the individual. Certain medications have been implicated in subacute lupus such as terbinafine, hydrochlorothiazide, calcium channel blockers, and drugs like naproxen or ibuprofen to name a few. Progression to the development of systemic lupus varies from 10-25 percent with some people having significant internal disease. [3]
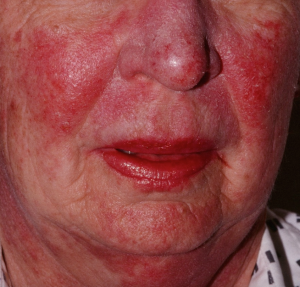
- Systemic Lupus Erythematosus: This is a systemic disease with multi-organ involvement most commonly affecting joints, skin, vascular system, lungs, kidneys and the central nervous system. People may experience a number of symptoms, such as but not limited to fever, arthralgias and myalgias, fatigue and weight loss, hair loss, butterfly rash on the face (especially after sun exposure), redness and edema particularly between joints on the hands and a photosensitivity rash (rash induced by the sun).
Typically, four or more of the following criteria must be present to make a diagnosis of systemic lupus. [2]
The Eleven Criteria
- Malar rash: butterfly-shaped rash across cheeks and nose
- Discoid (skin) rash: raised red patches
- Photosensitivity: skin rash as result of unusual reaction to sunlight
- Mouth or nose ulcers: usually painless
- Arthritis (nonerosive) in two or more joints, along with tenderness, swelling, or effusion. With nonerosive arthritis, the bones around joints don’t get destroyed.
- Cardio-pulmonary involvement: inflammation of the lining around the heart (pericarditis) and/or lungs (pleuritis)
- Neurologic disorder: seizures and/or psychosis
- Renal (kidney) disorder: excessive protein in the urine, or cellular casts in the urine
- Hematologic (blood) disorder: hemolytic anemia, low white blood cell count, or low platelet count
- Immunologic disorder: antibodies to double stranded DNA, antibodies to Sm, or antibodies to cardiolipin
- Antinuclear antibodies (ANA): a positive test in the absence of drugs known to induce it
References:
- Cohen, Bernard A. (2013). Pediatric Dermatology (4th ed., pp. 60-61). China: Saunders Elsevier.
- Lupus Research Alliance (2016). No Two Cases Are Alike. Retrieved February 12, 2017 from http://www.lupusresearchinstitute.org/lupus-facts
- Bolognia, Jean L., Jorizzo, Joseph L., Schaffer, Julie V., Callen, Jeffry P., Cerroni, Lorenzo, Heymann, Warren R., et. al. (2012). Dermatology (3rd ed., pp. 617-622). China: Saunders Elsevier.