Fifty million Americans suffer from autoimmune disease. Pemphigus is one type.
By Emily Jorge, DCNP, FNP-BC
According to the American Autoimmune Related Diseases Association (AARDA), 50 million Americans suffer from autoimmune disease. [1] Multiple literature define autoimmune disease as the body’s inability to differentiate between that which is foreign and that which is considered self. Inevitably, the body attacks its own tissues as a result.
In the world of skin, multiple autoimmune diseases abound, some of which we have heard of. Skin manifestations of lupus, rheumatoid arthritis, vitiligo, vasculitis, and alopecia areata are some common ones. A less commonly known autoimmune disease is pemphigus–when the body in the form of immunoglobulins and other cells attack the glue that holds our skin together. This glue is made up of proteins such as desmoglein and desmocollin.
The word pemphigus stems from pemphix, a Greek term meaning blister or bubble. [2] While there are three main divisions pemphigus can be divided into, we will discuss six types:
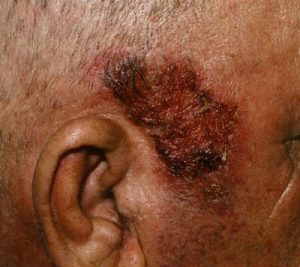 Pemphigus Vulgaris: Chronic large blisters called bullae first appear 60% of the time in the mouth or at the site of skin injury. Other common sites are the skin folds, scalp, and genitals. These large fluid filled bullae rupture easily causing painful open sores and crusted erosions. There are three subtypes: mucosal, mucocutaneous (mixture of skin and mucosal surfaces), and cutaneous (skin only). Death rates are highest among the mucocutaneous type. Because of the missing “glue” between cells in the superficial layers of the skin, slight pressure can move the tissue laterally. This is called a positive Nikolsky sign when this happens. There are other diseases that can be associated with pemphigus such as a neuromuscular disease called myasthenia gravis and thymus disease. Malignancy can occur at a higher rate among those with pemphigus. This is an extremely rare disorder in childhood. Untreated disease can be fatal. Treatment is continued until pemphigus antibodies disappear from the blood. [2]
Pemphigus Vulgaris: Chronic large blisters called bullae first appear 60% of the time in the mouth or at the site of skin injury. Other common sites are the skin folds, scalp, and genitals. These large fluid filled bullae rupture easily causing painful open sores and crusted erosions. There are three subtypes: mucosal, mucocutaneous (mixture of skin and mucosal surfaces), and cutaneous (skin only). Death rates are highest among the mucocutaneous type. Because of the missing “glue” between cells in the superficial layers of the skin, slight pressure can move the tissue laterally. This is called a positive Nikolsky sign when this happens. There are other diseases that can be associated with pemphigus such as a neuromuscular disease called myasthenia gravis and thymus disease. Malignancy can occur at a higher rate among those with pemphigus. This is an extremely rare disorder in childhood. Untreated disease can be fatal. Treatment is continued until pemphigus antibodies disappear from the blood. [2]
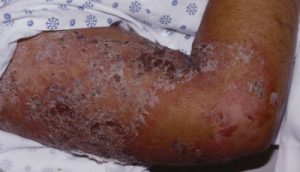 Pemphigus foliaceus: This is considered more of a subtype of pemphigus vulgaris. Although it may be seen in any age group, it is mostly found in older adults. While oral lesions may be common in pemphigus vulgaris, they are rare in pemphigus foliaceus. Commonly affected areas include sun exposed areas such as the scalp, upper chest, abdomen and back. Blisters may be found that easily form into multiple plaques and often it is misdiagnosed as impetigo. When a drug such as nifedipine, captopril, or penicillamine cause pemphigus foliaceus, stopping the offending drug will clear up the rash 50% of the time. [3] There are two subtypes of pemphigus foliaceus:
Pemphigus foliaceus: This is considered more of a subtype of pemphigus vulgaris. Although it may be seen in any age group, it is mostly found in older adults. While oral lesions may be common in pemphigus vulgaris, they are rare in pemphigus foliaceus. Commonly affected areas include sun exposed areas such as the scalp, upper chest, abdomen and back. Blisters may be found that easily form into multiple plaques and often it is misdiagnosed as impetigo. When a drug such as nifedipine, captopril, or penicillamine cause pemphigus foliaceus, stopping the offending drug will clear up the rash 50% of the time. [3] There are two subtypes of pemphigus foliaceus:
Pemphigus erythematosus: Red crusted lesions appear on the nose and cheeks similar to the “butterfly rash” of lupus. This is a localized version of pemphigus foliaceus. People with this are urged to always use sunscreen when outside.
Pemphigus herpetiformis: This rare subtype presents often as crusted lesions associated with severe itching. Sometimes hives can be seen early on then tense blisters and erosions. It typically is benign and forms on the trunk or portions of extremities closer to the trunk. It doesn’t usually show up on mucous membranes. [4]
Pemphigus Vegetans: Vegetative typically means there is an outgrowth where there are multiple papules forming a mass of tissue that projects outward. Only occurring in 1-2% of pemphigus vulgaris cases, it usually is found in people ages 40-50 years. There is a severe type called the Neuman type and a milder type called Hallopeau type. Pemphigus Vegetans arises most of the time in skin folds or in the mouth. A classic tongue finding called a cerebriform tongue, because it resembles the brain in texture with multiple crevices, is a characteristic feature. [2]
IgA pemphigus: Occurring mainly in middle age to older adults, this type of pemphigus has specific autoantibodies called IgA (immunoglobulin A) attacking the glue that holds the skin together, instead of IgG (immunoglobulin G). Two types based on their cellular findings have been identified. The first is called subcorneal pustular dermatosis type. Here the autoantibodies are attacking just the upper portion of the epidermal layers of the skin. In the second type, intraepidermal neutrophilic type, autoantibodies are found attacking throughout the entire epidermis of the skin. The condition is benign and may wax and wane for 5-8 years. However, it is very difficult to distinguish the subcorneal type from another rash called subcorneal pustular dermatosis. A special biopsy performed by your provider called DIF can help. [2]
Drug-Induced pemphigus: Drug reactions can mimic just about any skin disorder and pemphigus is no exception. Penicillamine and captopril are the main culprits, however, there are others. Beta blockers, ceftazidime, progesterone, rifampin and sulfasalazine are others that evoke a pemphigus-like drug reaction. Most, but not all, patients go into remission after the drug is discontinued. [2]
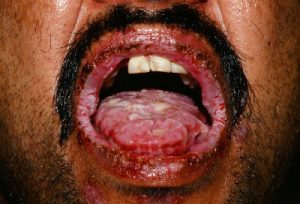 Paraneoplastic pemphigus: Painful ulcerations in the mouth or other mucosal surfaces with crusting of the lips may occur, typically due to a malignancy somewhere else in the body. The most common associations are non-Hodgkin lymphoma, chronic lymphocytic leukemia, Castleman tumor (abnormal overgrowth of cells of the lymph system), sarcoma (malignant connective tissue tumor), and thymoma (malignant cancer cells form on the surface of the thymus). Many times a blistering rash will be on fingers and hands, clinically differentiating it from pemphigus vulgaris. Severe eye irritation and lung involvement is also frequent in paraneoplastic pemphigus. There is a paraneoplastic pemphigus serum antibody screen test, but can be negative even when a tumor is present. [2]
Paraneoplastic pemphigus: Painful ulcerations in the mouth or other mucosal surfaces with crusting of the lips may occur, typically due to a malignancy somewhere else in the body. The most common associations are non-Hodgkin lymphoma, chronic lymphocytic leukemia, Castleman tumor (abnormal overgrowth of cells of the lymph system), sarcoma (malignant connective tissue tumor), and thymoma (malignant cancer cells form on the surface of the thymus). Many times a blistering rash will be on fingers and hands, clinically differentiating it from pemphigus vulgaris. Severe eye irritation and lung involvement is also frequent in paraneoplastic pemphigus. There is a paraneoplastic pemphigus serum antibody screen test, but can be negative even when a tumor is present. [2]
References:
- American Autoimmune Related Diseases Association. (2017). Autoimmune Statistics: Autoimmune Disease Fact Sheet. Retrieved March 8, 2017 from https://www.aarda.org/autoimmune-information/autoimmune-statistics/
- Bolognia, Jean L., Jorizzo, Joseph, & Rapini, Ronald. (2012). Dermatology (3rd ed., pp. 469-474). China: Saunders Elsevier
- DermNet New Zealand. (2003). Pemphigus foliaceus. Retrieved March 12, 2017 from www.dermnetnz.org/topics/pemphigus-foliaceus/
- Stojkovic-Filipovic, Jelena, Lekic, Branislav, Milcic, Danijela, & Milinkovic, Mirjana V. (2016). Pemphigus herpetiformis—A case report of a rare form of pemphigus and review of literature. Vojnosanit Pregl, 73(10): 967-972. Retrieved March 12, 2017 from www.doiserbia.neb.rs/img/doi/0042-8450/2016/0042-84501600044S.pdf